Endometriosis: Classification, symptoms, diagnosis, treatment
Endometriosis is a chronic gynecologic disease in which the endometrial glands and stroma grow outside the uterine cavity. Causes, symptoms, diagnosis and treatment.
This article is for informational purposes only
The content on this website, including text, graphics, and other materials, is provided for informational purposes only. It is not intended as advice or guidance. Regarding your specific medical condition or treatment, please consult your healthcare provider.
Vulvitis is an inflammation of the vulvar tissues that generally occurs secondary to various vulvar conditions. The disease tends to affect the labia minora and majora, clitoris, mons pubis, and vestibule of the vagina.
Vulvitis is common among premenarchal girls and postmenopausal women. Both groups have low estrogen levels that may cause the vulvar tissues to become thin and dry. Thin vulvar tissues, in turn, are more prone to injuries and infections.
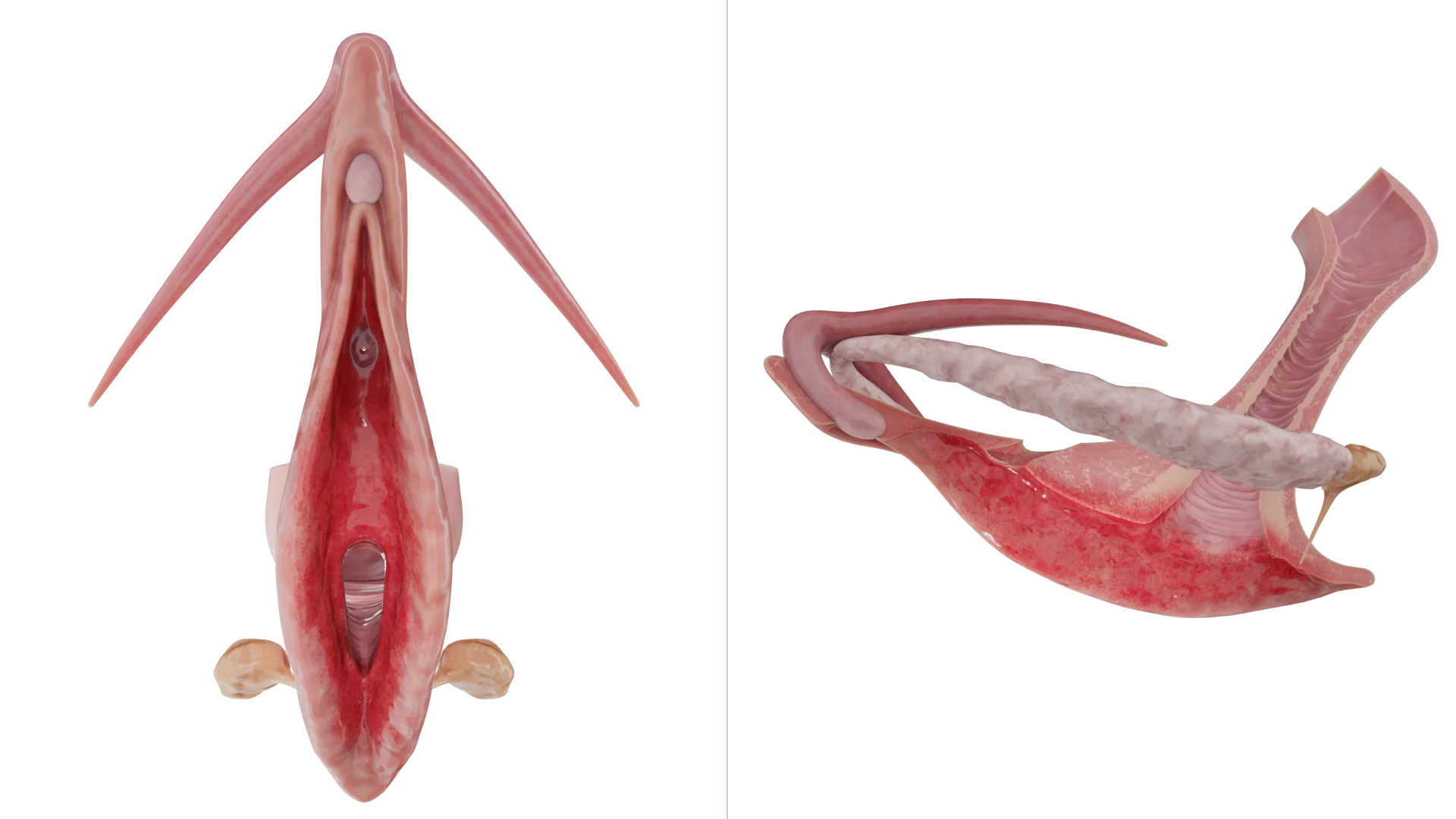

Note that generally, inflammation is not limited to the vulva but spreads further to the vagina; such cases are described as vulvovaginitis.
Besides an infectious nature, vulvitis may develop as an idiopathic condition. For instance, one of the forms is granulomatous vulvitis, which manifests as chronic, painless edema of the genitalia and shows histological signs of granulomatous inflammation.
One more distinct category among vulvar conditions is vulvar dermatoses:
In vulvitis, infectious agents typically belong to the opportunistic pathogenic microflora. In approximately 90% of cases, vulvitis is associated with Candida albicans. The remaining reports indicate involvement of E. coli, Staphylococcus epidermidis, group B Streptococcus, Enterobacterales, etc. The list of bacterial pathogens is not limited to the species mentioned above and may also include Neisseria gonorrhoeae, Trichomonas vaginalis, and Chlamydia trachomatis.
The most common viral agent is the herpes simplex virus.
Occasionally, vulvitis may develop due to bacteria causing tuberculosis and diphtheria. However, such instances are rare.
Note that infections only develop when vulvar tissues are injured by a specific factor.
Vulvitis may develop due to certain conditions when the integrity of the skin and mucosa of the external genitalia is compromised. These include:
Patients may not have any specific complaints but experience:
These lesions may be of normal skin color or develop reddish, whitish, brownish, or black shades.
In cases of vulvovaginitis, patients may also observe an abnormal foul-smelling discharge.
Chronic inflammation in the vulvar region may induce the following:
In such instances, patients report persistent dyspareunia (painful sexual intercourse) and dysuria (painful or uncomfortable urination).
Vulvar lichen sclerosus mainly affects the labia minora and majora, prepuce of the clitoris (clitoral hood), and perianal region. Generally, the vagina remains intact. Around 10% of patients experience extragenital lesions.
Upon examination, the tissues look pale and often atrophic. Atypical variations may present with hyperkeratosis.
As a pathognomonic symptom, purpura (or bruising, ecchymosis) is also observed. Compromised morphology of the external genitalia leads to resorption of the labia minora and/or midline fusion. Furthermore, the clitoral hood may become fused with an otherwise unaffected clitoris. Erosions are common; lichenification and hyperkeratosis may be occasionally observed. Note that these signs are not typical for vulvitis and may be indicative of vulvar intraepithelial neoplasia.
The changes may either be localized (generally on the clitoral hood) or include the perianal region and resemble a figure of 8.
Depending on clinical manifestations, vulvar lichen planus may be classified as follows:
Lichen simplex chronicus vulvar is frequently associated with atopic eczema or psoriasis. Continuous scratching leads to lichenification, meaning thickened, slightly scaly skin that has a pale or earthy tint. Clinically, it appears as erythematous inflammation with poorly defined edges; it might present with fissures. The skin appears very dry (xerosis), slightly scaly, and becomes thickened and lichenified due to chronic scratching.
Irritant contact dermatitis typically appears as coalesced lesions and is limited to the area that has been in direct contact with the irritant.
Unlike the irritant form, the skin affected by allergic contact dermatitis may present with macular lesions; the lesion edges are less defined and cover a larger surface than the contact area with the suspected allergen. Signs and symptoms of allergic contact dermatitis typically show 48-72 hours after the allergen contacts the previously sensitized skin. In severe cases, the skin of the genitalia becomes extremely inflamed and edematous; sometimes weeping, blisters, and erosions may develop.
Seborrheic dermatitis typically manifests as slightly pink, shiny, poorly outlined patches with a thin whitish scale. Skin alterations may affect the pubic region, inguinal grooves, anal region, and vulva. Lichenification is also typical for the condition. The affected areas often bear excoriations, and pubic hair loss may be observed.
Vulvar psoriasis generates clearly defined, brightly colored erythematous plaques that appear symmetrical and are found on the labia majora. The lesions may spread to the inguinal grooves and perianal skin. Fissures may be observed, whereas scaling is rare. Other body regions, such as the scalp, umbilicus, or nails, also tend to be involved.
Clinical manifestations of a squamous intraepithelial lesion (earlier referred to as vulvar intraepithelial neoplasia) may vary. The condition may generate white or erythematous, pigmented, often wart-like plaques. Multifocal lesions are often nonresponsive to treatment. Lesions may be hyperkeratotic, erosive, or ulcerated. They are commonly found around the clitoris, labia minora, and vaginal introitus, as well as the internal surface of the labia majora. The perianal area and perineum are rarely affected.
Vulvar dermatosis is treated locally with glucocorticosteroids.
| Condition | Treatment | Options |
|---|---|---|
| Vulvar lichen sclerosus | Clobetasol propionate |
Mometasone furoate |
| Vulvar lichen planus | Clobetasol propionate Vaginally: clobetasol propionate or prednisolone as a suppository |
Locally: calcineurin inhibitors (under dermatological supervision) |
| Vulvar eczema, atopic eczema, contact dermatitis, seborrheic dermatitis |
Emollients and soap substitutes. Mild and moderate conditions may be treated with topical steroids once daily. Irritants should be avoided |
In cases of severe inflammation or lichenification, clobetasol propionate may be used. Sedatives. Antihistamines |
| Vulvar psoriasis | Topical steroids | Vitamin D analogues. Coal tar gels and ointments |
1. What is vulvitis, and what are its causes?
2. What are the typical clinical manifestations and symptoms of vulvitis?
3. What is candidal vulvitis, and how is it treated?
4. How can vulvitis be contracted, and is it transmissible to men?
5. How long is the treatment for vulvitis, and can it resolve on its own?
6. How does vulvitis manifest in children?
7. What distinguishes vulvitis from “thrush”?
8. Can vulvitis be treated during pregnancy?
9. How does vulvitis present in pregnant women?
References
1.
VOKA 3D Anatomy & Pathology – Complete Anatomy and Pathology 3D Atlas [Internet]. VOKA 3D Anatomy & Pathology.
Available from: https://catalog.voka.io/
2.
Workowski KA, Bachmann LH, Chan PA, Johnston CM, Muzny CA, Park I, Reno H, Zenilman JM, Bolan GA. Sexually Transmitted Infections Treatment Guidelines, 2021. MMWR Recommendations and Reports [Internet]. 2021 Jul 22;70(4):1–187.
Available from: https://doi.org/10.15585/mmwr.rr7004a1
3.
Denning DW, Kneale M, Sobel JD, Rautemaa-Richardson R. Global guideline for the diagnosis and management of vulvovaginal candidiasis. Mycoses [Internet]. 2023.
Available from: https://doi.org/10.1111/myc.13574
4.
Gonçalves B, Ferreira C, Alves CT, Henriques M, Azeredo J, Silva S. Vulvovaginal candidiasis: Epidemiology, microbiology and risk factors. Crit Rev Microbiol. 2022;48(2):195-214.
5.
Pappas PG, Kauffman CA, Andes DR, Clancy CJ, Marr KA, Ostrosky-Zeichner L, et al. Clinical practice guideline for the management of candidiasis: 2023 update by the Infectious Diseases Society of America. Clin Infect Dis [Internet]. 2023.
Available from: https://doi.org/10.1093/cid/ciac803
6.
Sobel JD, Mitchell C, Nyirjesy P, Foxman B. Treatment of vulvovaginal candidiasis: Executive summary of the 2023 clinical practice guideline. Obstet Gynecol [Internet]. 2023.
Available from: https://doi.org/10.1097/AOG.0000000000005154
7.
Vieira-Baptista P, Pérez-López FR, López-Baena MT, Stockdale CK, Preti M, Bornstein J. Risk of development of vulvar cancer in women with lichen sclerosus or Lichen planus: a systematic review. Journal of Lower Genital Tract Disease [Internet]. 2022 Mar 11;26(3):250–257.
Available from: https://doi.org/10.1097/lgt.0000000000000673
8.
World Health Organization. WHO guideline for the treatment of vaginal discharge. Geneva: WHO Press; 2023.
9.
Mitchell C. Vaginitis: Diagnosis and treatment beyond bacterial vaginosis and candidiasis. JAMA. 2023;329(10):821-832.
10.
Nyirjesy P. Chronic vaginitis: Differential diagnosis and management. Clin Obstet Gynecol [Internet]. 2022.
Available from: https://doi.org/10.1097/GRF.0000000000000721
11.
Muzny CA. Aerobic vaginitis: An underdiagnosed cause of vaginal discharge. Clin Microbiol Rev. 2023;36(1):e00086-22.
12.
Pereyre S, Caméléna F, Hénin N, Berçot B, Bébéar C. Clinical performance of four multiplex real-time PCR kits detecting urogenital and sexually transmitted pathogens. Clinical Microbiology and Infection [Internet]. 2021 Oct 4;28(5):733.e7-733.e13.
Available from: https://doi.org/10.1016/j.cmi.2021.09.028
13.
Taylor SN. Mycoplasma genitalium: Emerging pathogen in non-gonococcal urethritis and cervicitis. J Clin Microbiol. 2023;61(4):e01888-22.
14.
Chanprapaph K, Seree-Aphinan C, Rattanakaemakorn P, Pomsoong C, Ratanapokasatit Y, Setthaudom C, et al. A real-world prospective cohort study of immunogenicity and reactogenicity of ChAdOx1-S[recombinant] among patients with immune-mediated dermatological diseases. Br J Dermatol [Internet]. 2023.
Available from: https://doi.org/10.1093/bjd/ljac001
15.
Wang CC, Rush SK, Uppal S, Rice LW, Spencer RJ. Trends in public- and industry-funded uterine cancer clinical trials and disability-adjusted life years from 2007 to 2019. American Journal of Obstetrics and Gynecology [Internet]. 2022 Jun 17;227(4):666–668.
Available from: https://doi.org/10.1016/j.ajog.2022.06.016
16.
Gaydos CA. Molecular testing for vaginitis: Current status and future directions. J Clin Microbiol. 2023;61(3):e01644-22.
17.
Campbell JR, Chan ED, Falzon D, Trajman A, Keshavjee S, Leung CC, et al. Low body mass index at treatment initiation and Rifampicin-Resistant tuberculosis treatment outcomes: an Individual Participant Data Meta-Analysis. Clin Infect Dis [Internet]. 2022.
Available from: https://doi.org/10.1093/cid/ciac315
18.
International Union against Sexually Transmitted Infections, World Health Organization. European guidelines for the management of vaginal discharge. Int J STD AIDS. 2023;34(3):135-148.
19.
Ambroggio L, Cotter J, Hall M, Shapiro DJ, Lipsett SC, Hersh AL, et al. Management of Pediatric Pneumonia: A Decade after the Pediatric Infectious Diseases Society and Infectious Diseases Society of America Guideline. Clin Infect Dis [Internet]. 2023.
Available from: https://doi.org/10.1093/cid/ciad385
Summarize article with AI
Choose your preferable AI assistant:
Link successfully copied to clipboard
Thank you!
Your message is sent!
Our experts will contact you shortly. If you have any additional questions, please contact us at info@voka.io